Lost in translation: Restoring Trust, Mission and Ethics in the Pharma Industry
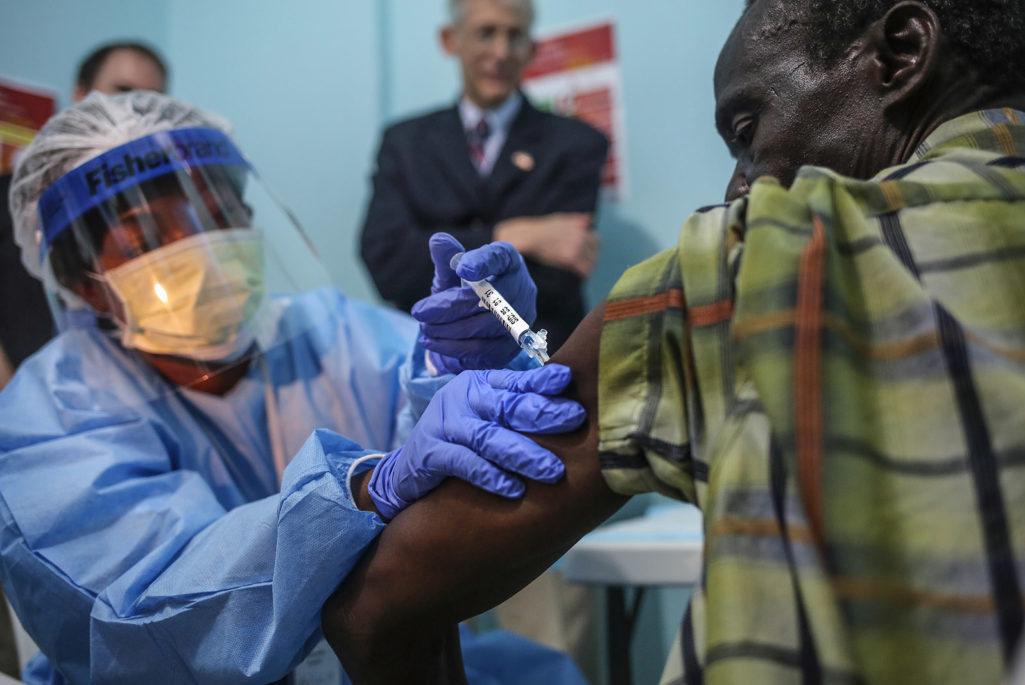
A nurse administers an injection on the first day of the Ebola vaccine trial being conducted at Redemption Hospital, formerly an Ebola holding center, in Monrovia, Liberia. The clinical research study is being conducted jointly by the U.S. National Institutes of Health and the Liberian Ministry of Health.
Photo by John Moore/Getty Images
The American public massively distrusts the pharmaceutical industry; the industry is ranked barely above tobacco companies and below Wall Street in terms of its honesty, ethics, and trustworthiness. However, a new tool has been developed to help the industry identify, signal and reform its ethics and trustworthiness issues.
The distrust of the pharma industry can be summarized with four numbers: 12, 70, 1 and 17:
- 12 percent of Americans trust pharmaceutical companies are honest and ethical.
- 70 percent think the companies put profits before people.
- Number 1 is what the industry used to be: the most admired business sector in the world.
- And about 17 years ago pharmaceutical companies still ranked among the top ten most admired companies.
To me, this drop in trust and esteem is a bit perplexing. The pharmaceutical industry represents a noble mission of healing the sick, treating the suffering, preventing disease, and saving lives. Somehow, this noble mission is not translating into practice or perception. This disconnect is proving costly for most stakeholders in healthcare.
Downsides of Distrust
Risks associated with distrust include exposure to irrational levels of reactive regulations; difficulty recruiting clinical trial participants; hesitancy by partners to collaborate with pharmaceutical companies; a difficulty in retaining and attracting employees; and litigation.
Distrust can also lower the value proposition around products, potentially creating hesitancy by healthcare organizations to reimburse and compensate for drugs and by patients to take them.
Distrust can erode the degrees of freedom an industry has to operate as it legitimately sees fit with its communities, stifle innovation, and ultimately hinder access to cures and therapies.
What is driving such distrust? One way to approach the trust gap and ethics concerns, is to divide them into five types of issues:
- Design of clinical trials—critics worry clinical trials are designed in biased ways to exaggerate the benefits of new drugs and minimize the appearance of harms—to sell more products.
- How trials are conducted—ethicists question, for example, whether companies test drugs for first world problems, like allergies and male pattern baldness, on people in developing countries who need clean water and tuberculosis medicines. They also question whether research participants can access medicines after the trials have ended.
- Transparency of results—studies have shown that less than half of all clinical trial results are publicly disclosed and those that are disclosed are often misleading and biased towards favorable results, further raising questions about the quality of our medical evidence.
- Marketing concerns—experts worry about the quality of medical education, when a significant portion of continuing medical education is funded by drug manufacturers.
- Accessibility—of medicines and vaccines for patients around the world.
Distrust can erode the degrees of freedom an industry has to operate, stifle innovation and hinder access to cures.
Restoring a Once Cherished Reputation
If we agree that loss of trust is a problem and that trust is an essential element for advancing innovation and global health, the question becomes: What can be done to appropriately repair the lost trust and the industry’s relationship with its communities? The pharmaceutical industry is not the first industry to suffer from quality management and reputational problems. The food, hospital, education, real estate, diamond, automobile and countless other industries have grappled with quality and reputational challenges.
These industries all turned to accreditation, certification, rating or auditing systems (multipronged) to assess, improve, and demonstrate the quality of their services, processes, and products. For example, the Kimberly certification program was started to prevent diamonds from being converted from symbols of love to symbols of bloodshed and conflict; the Flipper Seal of Approval that helped the canned tuna industry address concerns that their fishing nets were harming dolphins; the Rainforest Alliance and Forest Stewardship Council that helped set environmental standards for timber products; car safety rating labels; and the Dow Jones Sustainability Index.
These systems help increase transparency, accountability, stakeholder confidence and awareness of best practices in companies. Benchmarking based on big data in a sense provides free consulting to companies, and all stakeholders for that matter, on critical performance indicators. If built properly, these ratings systems can create knowledge exchange platforms and learning opportunities for everyone.
In 2009, an index for the pharmaceutical industry began to be developed under the auspicious of the nonprofit Bioethics International, with support from Harvard University, Duke University, The Susan G. Komen Foundation, and The Raskob Foundation. A pilot index is now finished that ranks large drug companies and new medicines and vaccines on their transparency. The index prioritizes the topic of clinical trial transparency because (1) companies were comparatively confident they were doing a good job in this area, (2) there were public data to measure performance, (3) the issue is fundamental to reforming other integrity challenges, and (4) it represents a serious public health and human rights challenge. Moreover, trial transparency is critical for:
- The quality and accuracy of medical evidence, prescription guidelines, and medical care—all of which are based on clinical trial information
- Speeding healthcare innovation and conserving research resources, because scientists can learn from prior scientific studies and avoid repetition
- Containing drug costs
- Protecting and respecting human research subjects
- Building a trustworthy healthcare innovation sector
Some companies scored well on the metrics. Others show a lot of room for improvement. However, now all ranked companies have a clearer understanding of how they are performing relative to their own institutional commitments and policies, relative to their peers, relative to ethics standards, and relative to the standards of their various constituencies.
The first results of the index will be published in a forthcoming medical journal. Meanwhile, we’re already seeing evidence that the industry is taking the results seriously. Many companies scoring lower on the index have reached out to us to understand the exact root causes of their low transparency (something we can show them with our data) and are evaluating how to improve their policies and practices. High scoring companies are able to use the index as a vehicle for defining what ethics and best practices can, should and do look like. And, we all slowly realize together that positive change is possible, and in fact already happening.




