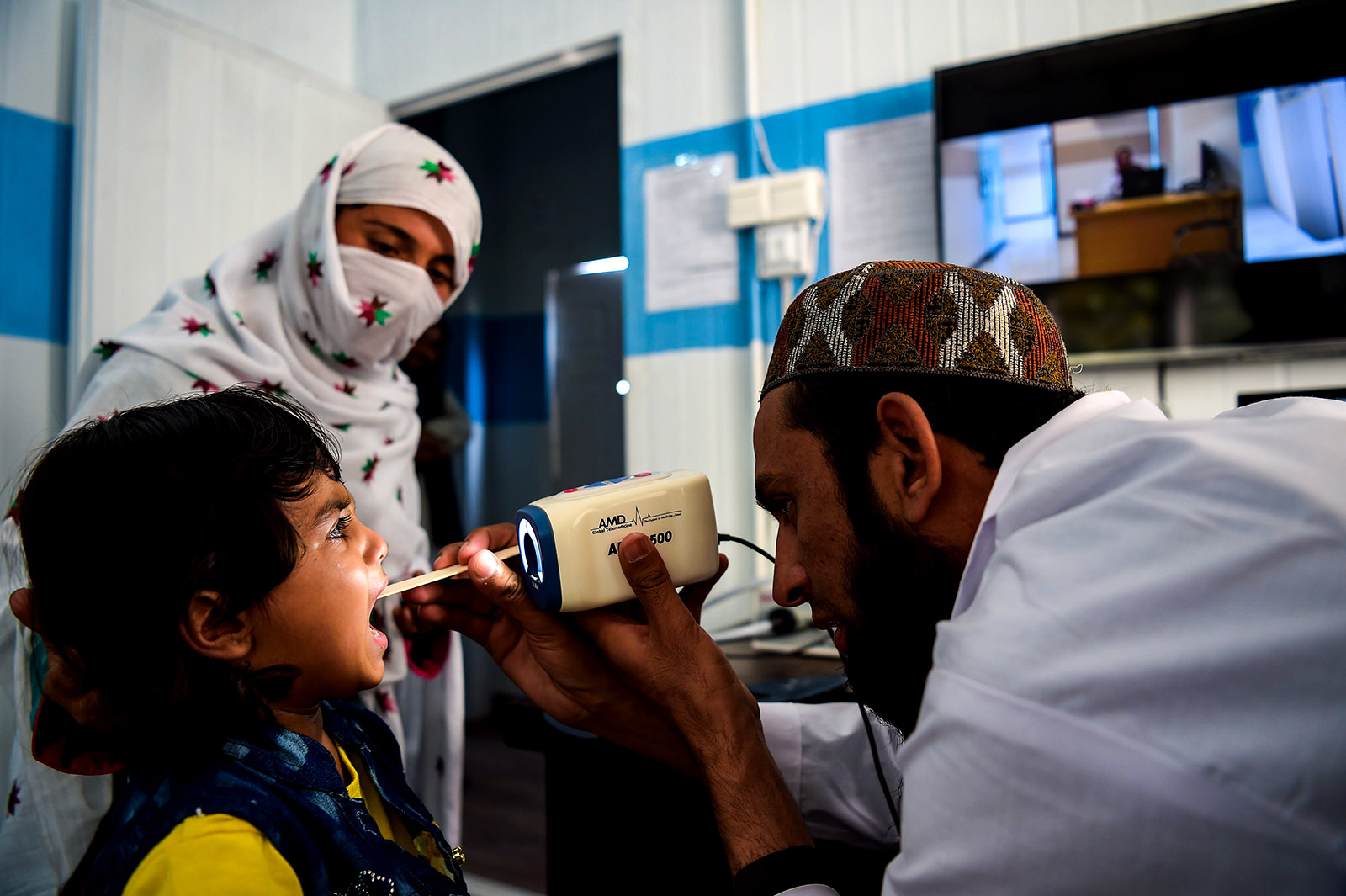
A paramedic in Pakistan checks a child's throat at a telemedicine online treatment center.
Photo: Aamir Qureshi/AFP/Getty Images
Technology offers huge opportunities for broad social benefit in public health care—particularly in the area of telehealth, which has the ability to deliver long-distance health care. BRINK News spoke to Rishi Madhok, the CEO of BitMED, a company that provides free health care to underserved communities in places as far apart as the Pacific Northwest and Mongolia.
BRINK: What exactly is telehealth?
Rishi Madhok: Telehealth refers to remote care—doctors and patients interacting with each other—whether it’s through a computer, an iPhone, or an Android app, or through remote consultation via email or a phone call.
Traditionally, medicine just takes whatever the current technology is and sticks it between the patient and doctor. But if you just take a video camera and stick it between a patient and doctor, I don’t believe you have actually improved care. I think you’ve actually made things a lot harder, because you’ve taken the patient-doctor interaction, where it’s already quite hard for information to be transacted, and now stuck a video camera or an audio telephone call in between, where data gets lost and call quality gets lost.
BRINK: So which areas of health care is telehealth working best in?
Dr. Madhok: The type of care that can be developed and given over this type of technology has really excelled in primary care, urgent care, and what I like to think of as referral services. The other area that has seen a lot of great success is essentially providing specialty services from provider to provider. There have been great advances in telestroke care. Stroke specialists are a scarce resource, but strokes are common, so the ability for an ER doctor to engage a teleneurologist quickly and efficiently helps guide the patient care early. If you can deliver the effective and right care more quickly in the setting of a stroke or a neurological emergency, you’re helping that patient’s long-term outcome to better restore their function.
BRINK: What is BitMED’s niche in this space then?
Dr. Madhok: Our view of health care, and telehealth specifically, is that we use it as a way to engage our users in a form of health care that they’re used to: I feel sick, I talk to a doctor. But the actual reality of BitMED is that we’re seeking health maintenance and health betterment. So, we use telehealth to efficiently engage our users with primary care doctors, family medicine, and emergency medicine doctors to help address the everyday needs—but also to help address long-term care plans with our patients.
We started out with just primary care and urgent care. We’ve expanded now to women’s health, quite a bit more preventative care, and engaging nutritionists from the platform. Our most recent pilots have revolved around mental health.
We’ve been focused on the U.S. markets, but also we felt that this technology was immediately addressable and scalable to emerging markets such as Rwanda and Kenya. We’re now moving into Ghana and then Asia: Myanmar, Thailand, Singapore and now Mongolia.
BRINK: You offer no-cost health care to these patients. How is that a sustainable business model?
Dr. Madhok: That’s a great question. In the current system, there’s always a cost: There’s the cost of getting in a car and driving, waiting in a waiting room. The average patient drives 10 to 85 miles to get to their physician. There’s an average wait time of 19 days for a general clinic appointment. The average cost is going to be anywhere from $50 to $500 in terms of engaging with your care.
It’s a catch-22. On one hand, as a person, you don’t want to be sick. But you also feel somewhat unfulfilled when you go to a doctor and they’re like, “well, you’re fine. It should clear up in a week. Just give it some time and we’ll follow up.” All this expense—and you walk away with nothing in hand. It’s something, as an emergency physician, that I’ve seen and felt many times.
When the patient is treated as a customer, that’s dangerous. Because when you’re treated as a customer, there’s a desire to give a product, and that’s why you see a lot of traditional tele-health care platforms over-prescribing—because the prescription becomes the product. You pay $20, you talk to a doctor, here’s a prescription. Did you need that antibiotic? Truthfully, no, and there’s very good studies to show that antibiotics and other medications have been overprescribed from tele-health care.
In the emerging market, there is a big opportunity for telehealth to be a bridge where health services tend to lag behind.
So, for BitMED we said, “listen, let’s take out all that friction. Let’s take out the hesitation for engagement from the patient side. Let’s take out the conflict the doctor feels from engaging the patient as an actual patient and person instead of a customer.” So the whole thing is no cost. We don’t bill insurance. We don’t do subscriptions. We don’t do copays. None of that.
BRINK: So where does your revenue come from?
Dr. Madhok: All of our work is fully subsidized and supported by the ability to derive insights and data products from what comes on the platform. If you look at attempts to develop a clinical decision support tool, why doesn’t it work? They feed it tons and tons and tons of data, but it still fails. Because they’re going to electronic health records that aren’t really meant for documentation of care. They’re definitely not meant for scientific development. They’re meant for billing.
What we offer is de-identified, aggregated data that has been structured for you to train your AI, to train your neuron network, to help you develop a pharmaceutical drug that has a good response profile to this very specific population.
And we don’t just give people no-cost health care. We incentivize the health care. When your data gets transacted as a member on our platform, you actually earn back what we call a BXM token. That token can be used for more goods and services on our platform—we’re working with hospitals, pharmacies, grocers, solar power companies to be able to accept this token so you can have a better life just by engaging in your health care. You get immediate benefits, but you also get long-term benefits as well.
BRINK: What are the organizations that pay for this data? Is it hospitals? Insurance companies? Where does the data go?
Dr. Madhok: Insurers can use this to help them in terms of where are the new markets for them to expand into? How do they understand risk adjustments for a 45-year-old male who has hypertension, diabetes, and what does that health care utilization look like? What’s the right insurance package for them?
We also take the de-identified data and create analyst reports and profiles. So if you’re a company looking to move into a new market and want to understand the disease penetrant of diabetes or HIV, we can provide you with those insights and reports to help you then move into a new market.
Then there’s academia. Coming from the academic world, patient engagement and involvement and acquisition of data are the biggest risks and represent 30 percent of the time of enrollment with any trial. We can help cut that down and save on cost tremendously and hopefully improve those outcomes.
BRINK: So you’re not actually providing the health care. You’re an intermediary to physicians, hospitals and so forth. Is that correct?
Dr. Madhok: BitMED is also the provider of health care. We have developed our own medical practice. It is a separate entity, completely blinded from how we make money. We have a collection of physicians, a pool of physicians, that we employ and pay, to provide direct care on our platform. Our AI bot engages the patient, asks them what’s going on, when did your headache start? Does anything make it better or worse? Do you have any of these associated symptoms like neck stiffness or fever? When it hits an end point to this logic, it transitions the care to our medical team.
The medical practice doctor then comes in, a family practitioner or emergency doctor, and they will look at the case and move to a treatment decision, either reassurance, a prescription if necessary, and, if needed, a referral to care and always a delivery of a treatment plan.
Then, the bot takes over the care again and basically asks the patient two questions at 48 hours. First: “How are you doing?” We want to make sure you are feeling better. Next, “Did we answer your question?” Because it gives the patient an opportunity to basically say whatever they felt may not have come to mind, or what they may not have had a chance to bring up in the clinical encounter. Maybe that patient had a grandmother who passed away from a brain tumor six months ago, and they want to make sure that their worsening headaches couldn’t be that. If there’s a negative response in those questions, the patient is offered again a clinical consult because they’re no cost. There’s no friction in bringing them back in.
BRINK: How has working in the developing world been a different experience to what you’ve been doing in the U.S.?
Dr. Madhok: Within the emerging market, there’s great opportunity because you have these kinds of leapfrog events within Africa and Asia. They leaped from phone lines underground, power lines above ground to solar power panels and solar connectivity. In Africa, there’s great adoption of mobile payment and mobile wallets, so there’s a strong understanding that one can engage with everyday goods and services from a mobile device.
For example, in Rwanda, their priority was nutrition and prenatal health. We said, “great, we’re happy to come to the country; give us two districts to start where we can help make an impact. Give us one in a densely populated city and the other in a more remote area.” Then we asked that they introduce us to a channel partner, so we have a private and a public partner in the health system. We basically hire local physicians to help support. We gauge academics to help provide local content. Also, we’re engaged with public health as well.
So we’re able to become a channel where people can push content through us. So you see in the emerging market the ability to be this bridge where health services tend to lag behind. Mobile technology and this connectivity has blossomed, and so we’ve been able to move through those markets extraordinarily well and get very readily available adoption.
This interview has been edited and condensed for clarity.




