The Massive Impact of COVID-19 on US Health Care
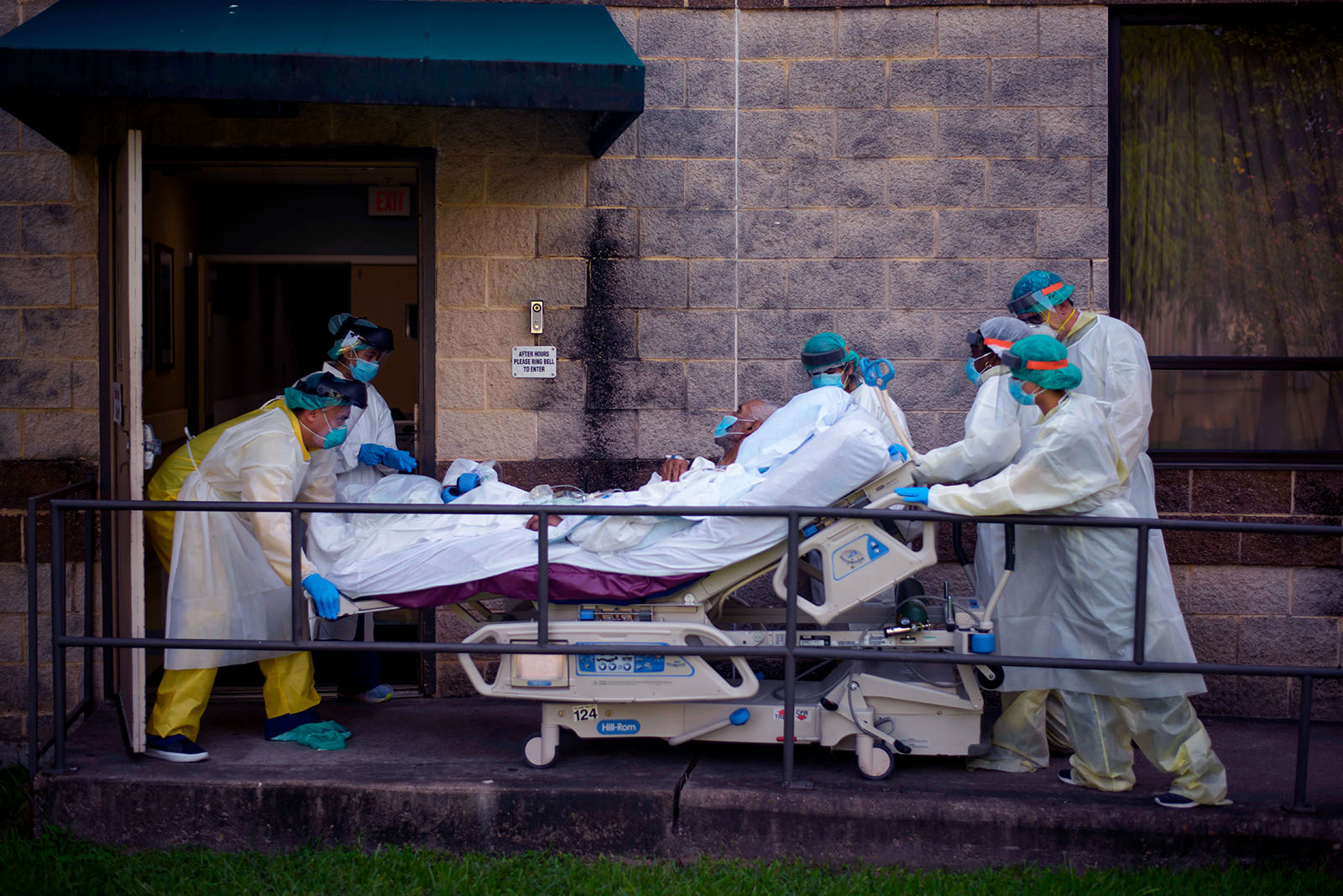
Health care workers move a patient at United Memorial Medical Center in Houston, Texas. Patients in Texas are more likely to experience surprise bills, since it has some of the highest rates of COVID-19 infections and hospitalizations.
Photo: Mark Felix / AFP via Getty Images
As COVID-19 continues to spread across the U.S., its impact on the U.S. health system is without precedent, with direct and indirect medical costs estimated to be in the hundreds of billions of dollars.
On an individual basis, cost estimates from the Peterson Center on Healthcare and Kaiser Family Foundation (KFF) range from between $10,000 to $90,000 per person depending on level of complications, ventilator use, etc.
The American Hospital Association estimates that American hospitals incurred more than $202 billion in losses between March 1st and June 30th — or more than $50 billion a month — from a combination of reduced revenue and increased costs.
Who is left to foot the final bill — and just how much of it — is one of the biggest unresolved questions, especially given the country’s unique patchwork system of health care delivery networks, range of insurance plans and variable policy priorities.
The Nasty Shock of ‘Surprise Billing’
Not only does America’s fragmented health care delivery system complicate billing and reimbursement, but insurer distinctions between in-network and out-of-network care often make it much more challenging. One example that is particularly relevant in the age of COVID-19 is so-called surprise billing, which often arises in an emergency situation when a patient has no ability to select the emergency room, treating physicians or ambulance providers.
According to the Peterson Center on Healthcare and KFF, for people in large employer plans, 18% of all ER visits and 16% of in-network hospital stays had at least one out-of-network charge associated with care in 2017.
While this varies by state, patients in Texas, New York, Florida and New Jersey were more likely to experience these surprise bills. As these states have some of the highest rates of COVID-19 infections and hospitalizations, the risk of actual costs becoming much higher is significant in these states, as well as more broadly across the country.
Furthermore, staggering and sustained unemployment levels warn of a much larger looming impact as the prospects grow that millions of Americans will soon be, if they aren’t already, without proper insurance coverage to afford care. In fact, data from over 800 hospitals in March found that levels of bad debt and charity care had already increased 13% over the previous year and is only expected to worsen with wider losses in coverage.
Temporary Legislative Interventions
Swift action by Congress and the easing of regulations by the Food and Drug Administration and Centers for Medicare & Medicaid Services have created a baseline level of support across COVID-19 testing and treatment. Collectively, $175 billion in provider relief was allocated via the Coronavirus Aid, Relief, and Economic Security Act in addition to the Paycheck Protection Program and Health Care Enhancement Act.
Meanwhile, most insurers, if not all, have activated emergency plans to ensure access to necessary testing and treatment options needed during this time. This includes waiving prior authorizations, diagnostic testing costs, in-network care, etc. However, the extent of these policies vary by insurer and state, as well as having different cut-off dates and levels of specificity.
Wide State-by-State Variance
While these responses have helped to provide economic and medical lifelines to millions of Americans and their families, bureaucratic and regulatory hurdles — and inconsistent levels of access to digital technology and care — threaten to exacerbate existing geographic and systemic disparities.
Despite these initial positive signals, it remains unclear how fluid and committed insurers, health authorities and Congress will continue to be on emergency medical priorities, financial relief provisions and supplemental insurance support as the pandemic rages on.
All stakeholders — patients, providers, insurers and policymakers — will have a role to play and a cost to pay as we learn from the virus.
The extent to which these commitments and policy protections extend through the end of year and into 2021 is up for debate, as the true effect of the COVID-19 burden and success of policy interventions become better understood.
The Virtual Doctor — Available Only to Some
Since the beginning of the COVID-19 pandemic, federal policymakers have enacted 31 changes to enable greater access to telehealth. As a country, we have witnessed an exponential rate of adoption of virtual doctors’ visits. However, many of these changes are temporary, and the digital divide between urban and rural communities persists, which has direct consequences on health care access and outcomes.
According to figures from the U.S. Federal Communications Commission, while 97% of Americans in urban areas have access to high-speed fixed internet service, the number falls to 65% in rural areas and barely 60% on tribal lands. To put that in perspective, an estimated 30 million Americans cannot fully reap the benefits of the digital age, particularly when it comes to their health care.
Supporting At-Risk Hospitals
The cancellation of elective surgeries as part of the statewide shutdown efforts — while good from a public health and COVID-19 mitigation effort to help flatten the curve and preserve critical hospital capacity — represents a huge revenue loss that will only further challenge the fiscal health of many rural health care centers.
In fact, in 2018 pre-pandemic, one-third of community hospitals in the U.S. had negative operating margins. So it’s perhaps unsurprising then that, according to the 2020 Rural Hospital Sustainability Index conducted by the consultancy Guidehouse, 25% of all U.S. rural hospitals are at a high-risk of closing unless their financial situations improve.
Notably, more than 46 million people, or 15% of the U.S. population, live in rural areas and, in general, tend to be older and sicker. Rural Americans experience higher rates of chronic conditions, are more likely to die from heart disease, cancer, chronic lower respiratory disease, and stroke, and are more likely to be uninsured.
Shaping a More Equitable System
While impact on insurers has seemed to be mild to date — with the postponement of many elective surgeries and slowdowns in doctor visits offsetting COVID-19 case costs — the full impact has yet to fully be realized. However, it does present opportunities to lead by example, use their immense financial and political leverage, as well as shape a more affordable and equitable health system.
Therapeutics and vaccines will be the ultimate key to ending the public health crisis. The coverage debate is already raging around the cost of Gilead Science’s coronavirus treatment remdesivir, with an estimated five-day cost of approximately $2,340 for governments and $3,120 for individuals with private insurance. As such, the pressure on insurers to ensure access and affordability of COVID-19 testing and treatment isn’t subsiding anytime soon.
To help mitigate some of this, insurers have the opportunity to reshape their perception as partners in health, improve a fragmented delivery system and prioritize universal access for improved care and outcomes.
Bridge the Digital Divide
In many ways, technological and policy prescriptions will be just as important to reduce disparities, improve outcomes, ensure equitable distribution of cost burden and protect the financial solvency of institutions most critical to community health.
Beyond extending COVID-19 protections and policies indefinitely through the end of the pandemic — as well as to cover out-of-network costs to avoid expensive surprise bills — insurers should begin to view broadband internet as a public utility and push for bridging the digital divide by increasing telehealth availability.
In the end, all stakeholders — patients, providers, insurers and policymakers — will have a role to play and a cost to pay as we learn from the virus, as well as our experiences with different approaches to improving access and reimbursement of care across the country and throughout our health systems.
How exactly the costs get distributed and paid will vary and become clearer with time but will nonetheless be a shared burden of sacrifice toward what we all hope will be a more equitable and fiscally secure health care system for all involved.




