What Can Employers Do to Impact Black-White Health Disparities?

There are still pronounced gaps as structural racism continues to adversely impact the health of Black Americans across multiple dimensions.
Source: Getty Images
Recent headlines, as well as longstanding research, underscore the reality that the health care system is not immune to the moral, economic or systemic consequences of racism. Employers now find they have a role in advocating for social justice and thus health equity — and as payers for care, they benefit from the economic and productivity gains inherent in more equitable access and improved outcomes.
The impact of employer efforts is crucial, given almost half of Americans receive employer-sponsored health insurance. This is a significant moment in time when we can work to eliminate health disparities, improve health outcomes and reduce health care costs.
What Causes Health Disparities?
Health disparities are not a function of individual or genetic differences but are influenced by systemic, social and economic factors. They are also amenable to change and improvement.
A disparity is a health outcome that is seen to a greater or lesser extent between populations, according to the CDC. Race or ethnicity, gender identity, sexual orientation, age, disability, socioeconomic status and geographic location all contribute to an individual’s ability to achieve good health. It is important to recognize the impact of social determinants — non-medical factors that influence health outcomes — on specific populations.
How Health Disparities Impact Business
The latest estimates indicate that social determinants of health may account for up to 80% of health disparities. This puts a significant financial strain on our health care system. Based on a Kaiser Family Foundation study, there is a $135 billion economic impact due to racial health disparities, including $93 billion in excess medical care cost and $42 billion in lost productivity.
A significant amount of these costs are borne by employers, who pay 82% of health care costs for employees and 70% of costs for families. The burden of absenteeism, presenteeism and employee turnover further impact employers’ bottom line. Take, for example, the impact of diabetes, which costs U.S. employers $20 billion annually in lost productivity. One of the most significant barriers for people with food-sensitive health conditions such as diabetes is lack of access to healthy foods. While 15% of the commercially insured population live in a low-access food area or food desert, only 1% of employers offer healthy food programs. Given the higher risk of diabetes onset for Black Americans, employers have a significant financial incentive to identify and address health disparities in their populations.
Racial Variance in Health Coverage and COVID’s Impact
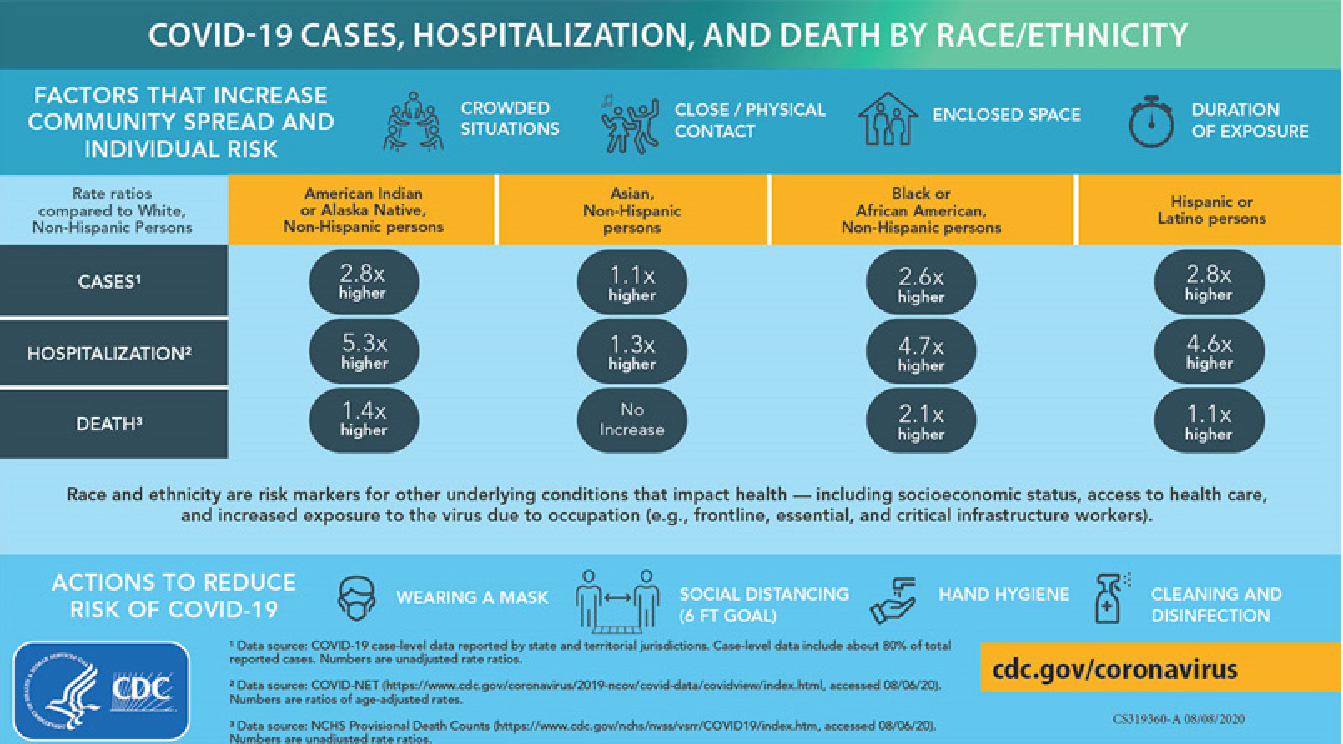
The pervasive disparities in health care coverage, access, quality and health outcomes between Black and white Americans are no secret — and the COVID-19 pandemic has further exposed and exacerbated these inequities. The chart below shows the large disparities related to COVID-19.
The death rate from infection was almost two times higher for Black Americans than for white Americans as of late January. As a result, Black Americans saw an overall decrease in life expectancy of 2.9 years as compared to 1.2 years for white people from 2019 to 2020.
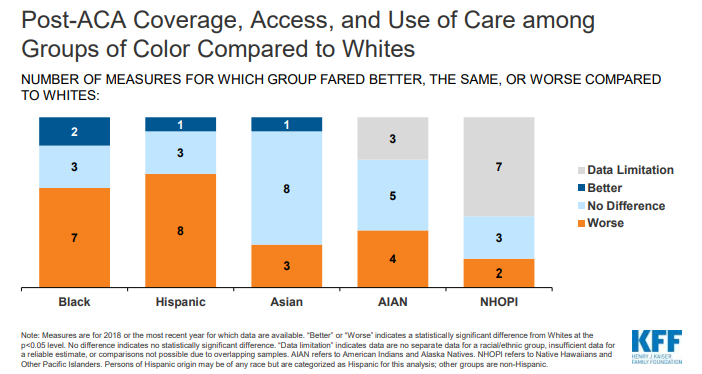
There had been progress in narrowing racial health disparities before these setbacks, such as improvements in access and insurance coverage under the Affordable Care Act. However, there are still pronounced gaps as structural racism continues to adversely impact the health of Black Americans across multiple dimensions. For example:
- Black Americans are more likely to die from heart disease than whites and have the highest mortality rate for all cancers combined compared with any other racial group.
- Black women are three times more likely to die of pregnancy-related causes than white women.
- Black men continue to experience health disparities even when controlling for higher educational attainment.
- Black babies continue to have the highest infant mortality in the nation.
- The 10 U.S. counties with the highest food insecurity rates have at least 60% Black population.
Employers Can Help — and Benefit from Employees’ Good Health
The good news is that employers have a distinct opportunity to confront health disparities through their central role in providing access to health insurance, benefits, education and targeted interventions for their employee populations.
There are several strategies that allow for collaboration between plan sponsors, health care providers and consultants to identify health disparities and strive for health equity, including:
Demographic data: Plan sponsors should send race and ethnicity data (as well as other demographic data) to the data warehouse.
Report on health disparities: Plan sponsors should request reports on existing quality metrics through the lens of race, ethnicity, gender and other demographics to see if there are disparities in key quality metrics, such as: preventive screening rates, chronic care guidelines and member experience. Engage data analytics teams to measure and understand the impact of health and well-being investments on employees and identify programmatic and behavioral sources of disparity that can be addressed through targeted action.
Develop and implement health equity initiatives: Based on the available demographic data that displays disparities, the plan sponsor, health plan, and consulting teams should work together to develop health equity initiatives, including key metrics, timeframes, accountability, and clinical guidelines. The implementation of these initiatives would be done by the health plan by educating, communicating and working with the providers in their networks regarding effective strategies regarding identified health disparities and the goals for health equity.
Monitor for improvement: Once the health equity strategies have been implemented, all stakeholders should receive reports on the progress using the previously identified health care quality metrics. There may need to be mitigating strategies to eliminate barriers and accelerate the achievement of health equity.
Communicate progress: It is important to transparently report on the progress of health equity initiatives with leadership, members, and other key stakeholders. This results in improved accountability that can accelerate health equity initiatives.
In summary, it will require a multi-stakeholder approach to address the $93 billion in excess medical care cost and $42 billion in lost productivity due to racial health disparities. Eliminating health disparities and achieving health equity involves all parties in the health ecosystem — employers, members, providers, carriers, vendors and consultants. Each plays a vital role in identifying and correcting systemic barriers, understanding social determinants of health and analyzing the metrics that define success.
We urge employers to look at the data, determine which metrics to use, and identify the target pace of improvement. As advocates for their communities and stewards of their employees’ interests, employers can be catalysts for change and take a leading role in defining a health care system that is affordable, accessible and fair for all.